Health & Dental Benefits
Health & Vision Coverage and Eligibility
San Francisco County IHSS Providers are eligible to enroll health and vision benefits through San Francisco Heath Plan Healthy Worker program. The coverage services include doctor visits, hospitalization, pharmacy, vision care and more. To qualify, state computer records must show you have worked and received payment for a San Francisco IHSS Recipient for 25 or more hours for the most current two consecutive months. This is an employee-based plan and does not cover dependents. For detailed information, please visit this website: www.sfhp.org/programs/healthy-workers/
Coverage Termination
Your health and dental insurance will terminate once state computer records show less than 25 worked/paid hours for 3 consecutive months in San Francisco County. The Public Authority will send you a warning letter 45 days before your insurance termination date. If your insurance is terminated, you must complete a new application form and meet the corresponding eligibility criteria before your insurance can start again. It is important to submit your timesheets on time and keep 25 or more paid/worked hours to prevent loss of coverage.
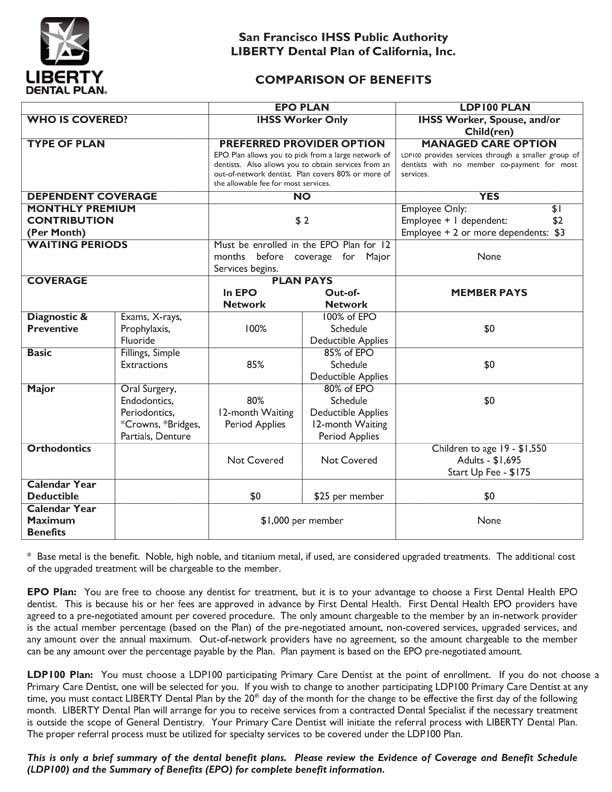
Dental Coverage and Eligibility
San Francisco County IHSS Providers are eligible to apply for dental benefits through Liberty Dental Plan and offers two plan options LDP100 and EPO. To qualify, state computer records must show you have worked and received payment for a San Francisco IHSS Recipient for 25 or more hours for the most current six consecutive months. Coverage can be for yourself and your dependents (depending on Plan Selection). For more information, please visit the Liberty Dental Plan website.
Applying for Coverage
Applications are automatically mailed only to newly eligible IHSS providers. If you are an IHSS Provider and meet the eligibility criteria and would like to apply, you can request an application by:
- Email: Send your email to benefits@sfihsspa.org with your full name and IHSS Provider ID number.
- Phone: Call 415-593-8125 and state your full name, IHSS Provider ID, phone number and detailed message.
- Applications are available in English, Chinese, Spanish, Russian, Tagalog, and Vietnamese.
Do you have more questions?
For detail information on Benefits, please review our Frequently Asked Questions below. If you still have questions email us at benefits@sfihsspa.org with your full name and IHSS provider ID number.